
Words matter. They settle deep in the psyche and impact our emotions, our beliefs – our overall outlook on things. This is never truer than with pregnancy and childbirth. All pregnant women, but especially a woman pregnant with her first child, is in new and unchartered space, and the people who surround her and the things they say impact her labor and first experiences as a mother.
Mind your words around a pregnant woman, and especially around a woman in labor.
Anthropologists and communication scholars write about two different paradigms of birth. Robbie Davis Floyd, Texas anthropologist and author, writes and lectures about the “technocratic” and “ecology” models of birth, arguing that there is freedom and space in the ecology model, but that in the technocratic model, the woman’s body is seen a machine and the baby as the product. Other researchers write about the “obstetrical” model, which includes the surgical training of obstetricians, versus the “midwifery” model, which includes the midwifery model of care and the importance of continuous support for the laboring woman. In each model you see a different lexicon of words.
For instance, who actually “delivers” the baby? It’s more common in the obstetrical/technocratic model to hear that the physician delivers the baby. But, the original use of the Middle English verb to deliver was passive. The Oxford Dictionaries site points out that “a woman was delivered of a child. When active use first arose, the midwife or doctor was the agent, and the woman the object: ‘they sent, and beg’d I would deliver her’ [1676].” In the beginning, deliver referred to the woman’s experience, whether liberation or rescue from the labor, or the woman freed from the burden of pregnancy. Next it moved to the active form that focused upon the woman’s agency in her birth experience, and today it has moved the main action to the attendant. “Dr. X delivered my baby.”
At the core, within the midwifery model, pregnancy is viewed as a natural life event for childbearing women. And out of that belief, words such as power, trust, love, empowerment, choice, and energy are often used to describe pregnancy and birth. There might be references to the power of nature/ birth or the power of the mother’s abilities in labor. Doulas and midwives use words such “rushes” or “waves” or “surges” to refer to a woman’s contractions, words that conjure up the image of a powerful ocean crashing against the seaside or strong electrical currents. And the midwife serves as facilitator, not director, in the mother’s natural life event.
By contrast, within the obstetrical model, pregnancy is viewed in terms of norms, with the male body as normal. Floyd takes this idea further by saying the woman’s body is seen as machine, the baby as product, and that pregnancy is something to be controlled: the doctor or midwife “deliver” the product through their control over the process with words like induce, intervene, and medicate. If the norm is to not be pregnant, then the labor needs to be actively managed. The action is focused not on the woman who is in labor, but on the staff who perform the management.
Somewhere in between is the reality of birth, right? There are times when a labor or pregnancy can move outside the norm of regular birth. While the woman’s body is designed for giving birth, labor can get complicated. In that case, the obstetrical model, with its emphasis on management and intervention and the provider in action, is a necessary model. But, given that approximately 90% or more (some researchers believe the more accurate number to be 95%) of women can give birth, can deliver their babies without intervention, why are obstetrical/technocratic words so commonly used? And why does it matter?
Women in labor are highly sensitive and intuitive. For example, if a woman is in active labor, moving quickly through the stages, and arrives at the hospital only to hear a nurse tell her that she won’t be giving birth until the next morning, guess what? The labor slows and the baby is born in the morning. If a soon-to-be-grandmother is anxious about the birth and present in the delivery room, the slightest slip of the tongue can have a negative impact on the laboring woman. If she says, “All the women in our family have cesareans, you’re no different,” the labor will be harder, the woman will have to fight against the negativity, and if not adequately prepared or supported, she might end up with a cesarean that may or may not have been needed if the words that surrounded her were positive and affirming. If a nurse tells a mother who is ready to push that the doctor needs to arrive to deliver the baby, the mother may lose her sense of agency over the delivery and the contractions may slow or the pushing become difficult.
The power of suggestion takes on a heightened meaning during birth.
In an article on the Birth International site, Abby Sutcliffe writes:
During labour, women are particularly alert to what is being said by caregivers. Even though she may look as though she is lost is concentration during contractions, the labouring woman will hear, often acutely, what is being said around her. She looks to the midwife for confirmation that she is doing well, particularly with handling the pain. A few well-chosen words of encouragement and support can be far more effective than [medication] in achieving relaxation and confidence in the labouring woman. The midwife at a birth has great influence on the woman’s reactions and impressions, so be careful not to introduce your own feelings and biases into the room. This woman is not a “poor thing” who won’t cope without you — she is a strong, innately capable woman uniquely designed for giving birth easily, safely and enjoyably. If you truly believe this then you won’t need to watch your language, you will already be consciously feeding this information back to through your language and responses.
Birth is a highly personal experience. Each laboring woman brings into the birthing room a personal story that includes the past birth experiences of the women in her family, her own hopes and fears, and any other past experiences that impact the natural process of birth, such as past sexual trauma or body image issues. Birth is a natural life event, a part of a women’s greater sexuality and biology. The words that she hears can help or heed her progress; it’s up to the people who surround her to make it the most positive and successful experience possible. Care providers: pay attention to the words you use around a pregnant or laboring woman. Family members and support team: think before speaking—everyone in the labor room should examine their own biases and experiences, their own fears, or even trauma that may not have been dealt with in the past. For the laboring woman, words really do matter.
Pregnant women deserve to feel supported and respected – empowered – to deliver her baby. No matter the final outcome—whether natural, or a birth with medication or a cesarean section—positive language in the birthing room puts the woman at the center of the action, so that she is in the best position to successfully deliver her baby.

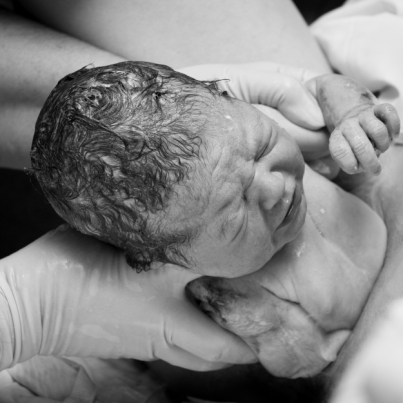
 Each woman arrives at a new pregnancy from a different starting point. One woman may have planned for months to get pregnant, taking vitamins, eating healthy, and exercising. Another might be classified as medically obese and is worried about how that will affect her pregnancy—should she lose weight or focus only on eating healthy? While yet another may have, not intending or wanting a pregnancy at the time, been drinking heavily or using illicit drugs. Of course, most women are somewhere in the middle. Ultimately it’s most important that a woman work at getting as healthy as possible, so that she and the baby have the best outcomes.
Each woman arrives at a new pregnancy from a different starting point. One woman may have planned for months to get pregnant, taking vitamins, eating healthy, and exercising. Another might be classified as medically obese and is worried about how that will affect her pregnancy—should she lose weight or focus only on eating healthy? While yet another may have, not intending or wanting a pregnancy at the time, been drinking heavily or using illicit drugs. Of course, most women are somewhere in the middle. Ultimately it’s most important that a woman work at getting as healthy as possible, so that she and the baby have the best outcomes. When a woman first discovers she’s pregnant, the birth can seem distant, an event that happens at the very end of pregnancy. There are nine months to get through first. She knows the birth will be something big, but it’s still a somewhat abstract idea—and maybe even a little scary. She can prepare by taking childbirth education classes or by asking her maternity care provider questions, but the real truth is that every birth is unique—and unpredictable.
When a woman first discovers she’s pregnant, the birth can seem distant, an event that happens at the very end of pregnancy. There are nine months to get through first. She knows the birth will be something big, but it’s still a somewhat abstract idea—and maybe even a little scary. She can prepare by taking childbirth education classes or by asking her maternity care provider questions, but the real truth is that every birth is unique—and unpredictable.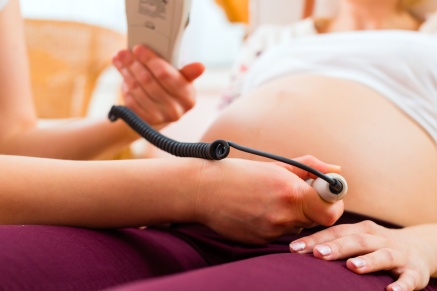
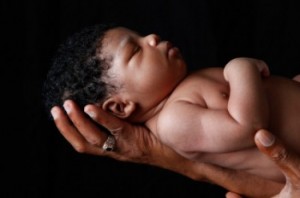
 The concept of the fourth trimester helps during this vulnerable time of change—looking at the early months through the eyes of the newborn, with empathy, helps the new parents in terms of setting expectations and making decisions. For instance,
The concept of the fourth trimester helps during this vulnerable time of change—looking at the early months through the eyes of the newborn, with empathy, helps the new parents in terms of setting expectations and making decisions. For instance, 



You must be logged in to post a comment.